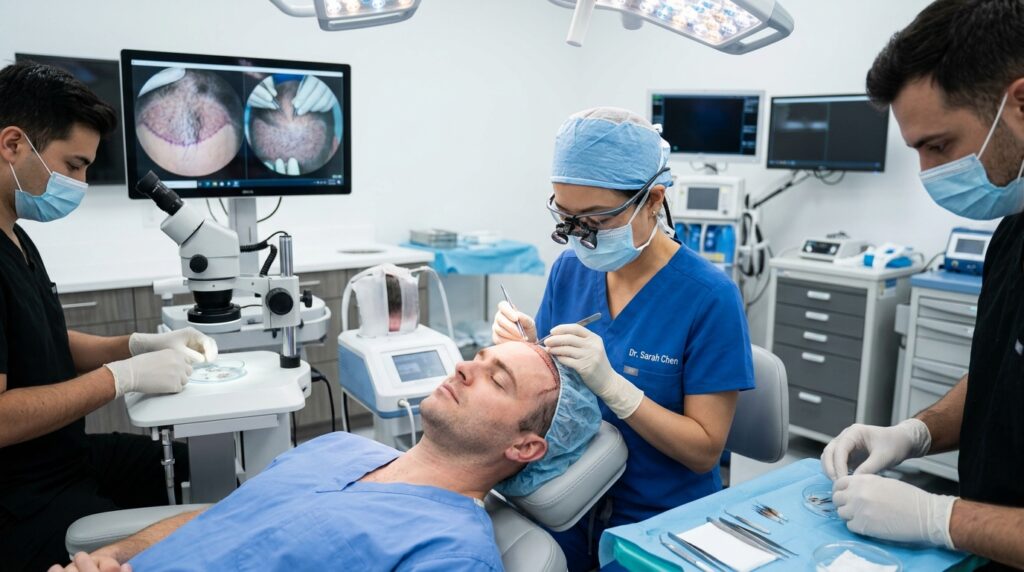
Hair loss affects approximately 50 million men and 30 million women in the United States alone. After more than two decades of practice in dermatology and hair restoration, I have witnessed the remarkable evolution of hair transplantation from a procedure that often produced unnatural results to today’s sophisticated techniques that deliver virtually undetectable outcomes. This article explores the current state of hair transplantation, helping patients understand their options and set realistic expectations.
The Science Behind Hair Loss
Before discussing treatment options, it’s essential to understand why hair loss occurs. The most common form is androgenetic alopecia, or pattern baldness, which affects both men and women. This condition is primarily driven by genetics and hormones, specifically dihydrotestosterone (DHT), a derivative of testosterone.
Hair follicles in certain areas of the scalp, particularly the crown and frontal hairline, contain androgen receptors that are sensitive to DHT. When DHT binds to these receptors, it triggers a process called miniaturization, where hair follicles progressively shrink, producing thinner and shorter hair until they eventually stop producing visible hair altogether.
Interestingly, hair follicles in the back and sides of the scalp are typically resistant to DHT. This characteristic is the foundation of hair transplantation—we can relocate these resistant follicles to balding areas where they continue to grow for a lifetime.
Modern Hair Transplantation Techniques
Follicular Unit Transplantation (FUT)
FUT, also known as the strip method, involves removing a thin strip of scalp from the donor area (typically the back of the head). This strip is then meticulously dissected under microscopes into individual follicular units—naturally occurring groups of 1-4 hairs. These units are then implanted into tiny incisions in the recipient area.
The advantages of FUT include the ability to harvest a large number of grafts in a single session (often 2,000-4,000+ grafts), making it ideal for patients requiring extensive coverage. The technique also allows for excellent visualization of the follicular units during extraction, potentially reducing transection rates. However, FUT does leave a linear scar in the donor area, which may be visible with very short hairstyles.
Follicular Unit Excision (FUE)
FUE has gained tremendous popularity over the past 15 years. This technique involves extracting individual follicular units directly from the scalp using small circular punches, typically 0.8-1.0mm in diameter. These grafts are then implanted into the recipient area, similar to FUT.
The primary advantage of FUE is the absence of a linear scar, allowing patients to wear very short hairstyles. The procedure is also generally less invasive, with faster healing time. However, FUE is more time-consuming and typically more expensive. In my practice, I often recommend FUE for patients who prefer to wear their hair very short or those who have tight scalps that make FUT more challenging.
Direct Hair Implantation (DHI)
DHI is a modification of FUE that uses a specialized implanter pen called a Choi pen. With this technique, graft extraction and implantation can occur almost simultaneously, and the direction, angle, and depth of each follicle can be controlled with precision. While DHI offers certain advantages in terms of control and potentially reduced handling of grafts, it requires significant expertise and may not be suitable for all cases.
The Hair Transplantation Process: What to Expect
Initial Consultation
A thorough consultation is paramount. During this visit, I assess the pattern and extent of hair loss, examine the donor area to determine density and quality, review medical history, and discuss realistic expectations. Not everyone is a suitable candidate for hair transplantation. Factors such as ongoing active hair loss, insufficient donor hair, certain medical conditions, or unrealistic expectations may preclude surgery.
I typically use the Norwood-Hamilton scale for men and the Ludwig scale for women to classify the degree of hair loss. This standardized assessment helps in treatment planning and allows for better communication about expected outcomes.
Pre-Operative Preparation
Preparation begins weeks before surgery. I advise patients to discontinue blood-thinning medications and supplements (aspirin, ibuprofen, vitamin E, fish oil) approximately two weeks prior to reduce bleeding risk. Alcohol and smoking should be avoided for at least one week before and after surgery, as both can impair healing and graft survival.
Some patients benefit from pre-operative finasteride or minoxidil treatment to stabilize hair loss and improve surgical outcomes. The hairline design is typically finalized on the day of surgery, with the patient’s input being crucial to ensure satisfaction.
The Procedure Day
Hair transplantation is performed under local anesthesia as an outpatient procedure. Most patients are awake and comfortable throughout, often watching movies or listening to music. A typical session lasts 4-8 hours depending on the number of grafts being transplanted.
The procedure begins with administering local anesthetic to both the donor and recipient areas. For FUT, the strip is harvested and the donor area is closed with sutures. For FUE, individual follicles are extracted. Throughout the procedure, the grafts are carefully kept in a chilled holding solution to maximize survival.
Creating the recipient sites is perhaps the most critical step. The angle, direction, and distribution of these incisions determine the naturalness of the final result. I pay meticulous attention to mimicking natural hair growth patterns, varying the angle and direction based on the area being treated.
Post-Operative Care and Recovery
The immediate post-operative period is crucial for graft survival. Swelling is common and typically peaks around the third day, particularly in the forehead area. This is normal and resolves within a week. Sleeping with the head elevated at a 45-degree angle for the first few nights helps minimize swelling.
The first hair wash typically occurs 7 days after surgery. I provide detailed instructions on gentle cleansing techniques to avoid dislodging grafts. Scabs form around each transplanted follicle and should be removed. Picking or scratching can damage the grafts.
Most patients return to desk work within 3-5 days. Strenuous exercise should be avoided for 2-3 weeks to prevent increased blood pressure that could compromise healing. The transplanted hairs typically shed within 2-4 weeks after surgery—this is completely normal and expected. This phenomenon, called shock loss, occurs because the trauma of transplantation causes the hair shaft to fall out, but the follicle remains viable and will produce new hair.
Timeline of Results
Patience is essential with hair transplantation. New growth typically begins around 3-4 months post-surgery, though some patients may not see initial growth until month 5-6. The hair initially grows in fine and thin, gradually increasing in caliber over time.
By 8-10 months, approximately 90-100% of the final result is visible. The complete outcome takes 12-18 months to fully materialize. I always counsel patients about this extended timeline during consultation to set appropriate expectations.
Success Rates and Realistic Expectations
When performed by experienced surgeons, hair transplantation has a very high success rate, with graft survival typically ranging from 90-95%. However, success isn’t solely measured by graft survival—the naturalness and aesthetic quality of the result are equally important.
It’s critical for patients to understand that hair transplantation redistributes existing hair rather than creating new hair. The procedure works best for patients with sufficient donor hair and realistic expectations. While we can achieve remarkable improvements in appearance and restore a natural-looking hairline, we cannot typically recreate the density of teenage hair.
Additionally, hair transplantation does not stop the progression of genetic hair loss. Patients with ongoing hair loss may require medical management (finasteride, minoxidil) to preserve their results, and some may benefit from additional procedures in the future as their hair loss pattern evolves.
Potential Complications and How to Minimize Them
Like any surgical procedure, hair transplantation carries potential risks, though serious complications are rare when performed by qualified practitioners. Common temporary side effects include swelling, numbness in the donor or recipient areas (usually resolves within 3-6 months), itching during healing, and minor infections (less than 1% of cases when proper sterile technique is used).
Shock loss—temporary shedding of existing hair in the transplanted area—can occur in 10-15% of patients. While distressing, this is usually temporary, with hair regrowing over the following months. Less common complications include cyst formation, poor graft growth, or unsatisfactory aesthetic results.
Minimizing complications begins with proper patient selection and continues with meticulous surgical technique and appropriate post-operative care. Choosing a board-certified dermatologist or plastic surgeon with extensive experience in hair restoration is perhaps the single most important factor in achieving successful outcomes.